 November 2013
November 2013
A New PICC Play — Microaccess Technique for PICC Insertion Through Strictured Vessels Offers Time and Financial Savings
By Sean Wiley, RPA/RA, RT(R)(CV); Jeffrey Vogel, MD; and Brandy Wiley, PA, BSRT(R)(CT)(MR)
Radiology Today
Vol. 14 No. 11 P. 32
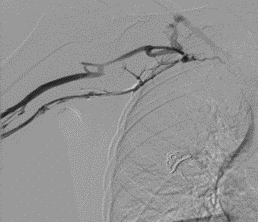
Figure 1
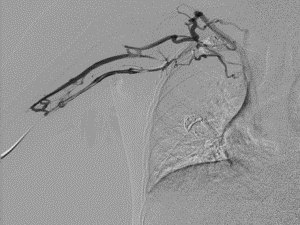
Figure 2
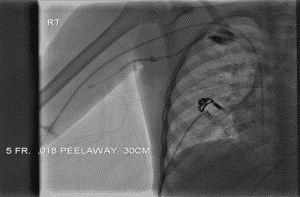
Figure 3
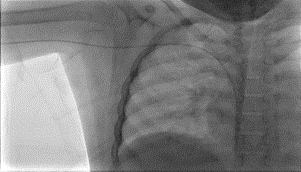
Figure 4
Figures 1 and 2 demonstrate midright subclavian vein stricture. Figure 3 demonstrates the tear-away sheath advanced through the venous stricture. The yellow arrow points to the distal tip of the tear-away sheath. Figure 4 demonstrates the PICC line in its appropriate position. The blue arrow points to the distal tip of the PICC line catheter.
Images courtesy of Sean Wiley, RPA/RA, RT(R)(CV)
Physicians face the challenge of what type of IV access lines to choose for their patients. That decision must consider several variables, including patient stability, the degree of infection, how long the access will be needed, and the number of lumens required. In patients with repeat venous access needs, venous strictures caused by previous use of multiple venous access devices are becoming a major issue and add another variable to the decision.
One of the most widely used IV access devices is a peripherally inserted central catheter (PICC). These plastic, silicone, polyurethane, or carbothane lines are inserted into the upper arm above the patient’s elbow and advanced into the superior vena cava above the heart. A PICC line usually is indicated for patients who need long-term chemotherapy, hyperalimentation, repeated administration of blood and blood products, repeated venous blood sampling, central venous pressure measuring, or fluid antibiotic administration.
Issues arise when patients repeatedly need a PICC line, resulting in a higher risk of venous thrombosis or venous strictures that make inserting the lines more difficult.
Several different methods have been used to ease PICC line insertion. One technique involves exchanging the 0.018-inch wire for a 0.035-inch wire so that a long dilator or peel-away sheath can be placed through the thrombosis or venous stricture. This allows the PICC line to be placed through the problem area and the tip location to be within the peripheral superior vena cava.
Another technique is to change the insertion sheath to a 4- or 5-French catheter and use a 0.035-inch Angled Glidewire to maneuver through the thrombosis or venous stricture to the superior vena cava. Once the catheter and wire are past the problem area, a 0.018-inch wire can be inserted through the catheter and the catheter removed to advance the PICC line.
Both ways are successful but increase time and expense of the procedure. We offer a case report of an alternative technique that may be used.
Case Study
A 7-year-old Caucasian male with cystic fibrosis presented for central venous access to allow the delivery of antibiotics. The ordering physician requested a PICC line. The patient previously had multiple PICCs in both upper extremities, and the inpatient PICC line team failed during the recent placement. The patient was referred to interventional radiology for a PICC line insertion attempt before possible placement of a tunneled central venous catheter.
Under ultrasound guidance, the right basilic vein was accessed with a 21-gauge microaccess needle from the Xcela PASV PICC line kit. Through the needle, a 0.018-inch wire was inserted under fluoroscopic guidance; however, the wire would not advance centrally past the mid right subclavian vein. The needle was removed from the wire, and the short 5-French sheath was placed. Contrast injection was performed and demonstrated a high-grade right midsubclavian venous stricture. The wire was reinserted, and the short sheath was exchanged for a 5-French X 30-cm (0.018-inch) tear-away sheath, which was placed over the wire and advanced to the stricture.
Due to the inability to cross the stricture, the 0.018-inch wire was manipulated to a larger collateral vein and advanced to the stricture. The 0.018-inch wire from the PICC line kit was removed, and a Galt Gold Nitinol 0.018-inch wire was advanced through the new pathway to the stricture. The wire then was advanced through the stricture and into the inferior vena cava. The tear-away sheath then was used to dilate the stricture using the Dotter technique, a method where the sheath is used to sequentially dilate the stricture to open it to the size of the tear-away sheath. The long length (30 cm) allows for easier placement of the PICC line through the tear-away sheath and into the distal superior vena cava. The tear-away sheath then was separated and removed, leaving the PICC line in the correct position within the distal superior vena cava.
Conclusion
Using longer microaccess introducer tear-away sheaths allows the operator to place the sheath past the area of thrombosis or venous stricture. The sheath becomes a conduit to allow easy placement of the PICC line through the sheath and into the appropriate location for distal tip placement. The microaccess tear-away sheath is available in 5-, 6-, and 7-French X 30-cm length with a 0.018-inch obturator (inner dilator).
In our experience, this technique has decreased operative time as well as expense. Exceptions include very tall patients or left-sided insertions where the 30-cm sheath length is not always long enough if the stricture is more central. Further follow-up to look at longer length tear-away sheaths vs. previously discussed techniques will need to be evaluated on these types of patients to determine ease of placement and decrease in time and cost.
— Sean Wiley, RPA/RA, RT(R)(CV), is the lead radiology extender at the University of Florida.
— Jeffrey Vogel, MD, is an assistant professor of radiology at the University of Florida.
— Brandy Wiley, PA, BSRT(R)(CT)(MR), is a recent graduate of the University of Florida physician assistant program.

