November 16, 2009
 Improving Emergency Department
Improving Emergency Department
and Imaging Throughput
By Marty Khatib, JD, RT(R)
Radiology Today
Vol. 10 No. 18 P. 42
Never before has there been such heated debate about the need for healthcare reform as we are experiencing now. In this firestorm, facilities still face highly challenging demands. They must distinguish their organizations by improving patient, staff, and physician satisfaction; raising the bar on quality; and redefining themselves as specialists within their communities.
With 50% of nonobstetric hospital admissions arriving through the emergency department (ED) and uninsured persons accounting for nearly 20% of all hospital-based ED visits, emergency medicine sits at the epicenter of the healthcare crisis.1,2 Despite this pressure, hospital administrators expect EDs to contribute to the overall financial health of the hospital, as they have in the past. This means that departments must continue to squeeze inefficiency out of their processes and eliminate bottlenecks that threaten the financial state of their hospital. Although many service lines support the ED, diagnostic imaging is arguably one of the most critical areas. According to the National Center for Health Statistics, imaging procedures are ordered for 44.2% of all emergency visits.
Effectively handling this large, unscheduled workload must include a timely radiology report with actionable information for the ordering physician. Often, this is only possible through effective load balancing, the art and science of adapting to fluctuations in volume. Radiology administrators and other administrators in the healthcare delivery system have experienced problems meeting these volume demands without some countermeasure of load balancing in place. At our four Catholic Healthcare West hospitals serving California’s Sacramento area, we have used teleradiology as an effective way to manage volume fluctuation and improve ED and imaging throughput.
Unbalanced Workload
A balanced workload is every imaging department’s dream. Administrators want to see patients flowing through the ED on schedule, just the right number of radiologists to interpret the studies in a timely manner, and no unexpected volume peaks or valleys to disrupt the process. Unfortunately, reality dictates a much different scenario. Specifically, the speed of delivering high-quality diagnostic imaging reports can be severely impacted by unexpected spikes in ED volume that overwhelm radiologists with urgent studies. This situation can be particularly acute during the evening hours, when fewer radiologists are typically available.
When an important service line such as imaging cannot keep up with demand, problems ensue and grow larger with each delay. Specifically, the time to diagnosis and treatment can be slowed, putting patients at risk. A domino effect keeps other ED patients in the waiting room longer and negatively impacts performance metrics such as ambulance diversion, length of stay, left without being seen, leaving before seeing an ED physician, leaving against medical advice, and missed registration.
Behind the unscheduled patients stalled in the ED, there’s often a line of scheduled procedures that are at risk of delay, further reducing overall throughput.
Finally, add the inevitable adverse impact to staff, physician, and patient satisfaction—not to mention lost revenue—and you have an imaging department that is suffering under its inability to effectively navigate a sudden demand for emergent interpretations.
Ideally, imaging managers have several options to help optimize patient flow. For example, strategic scheduling can increase productivity from technology advancements such as enterprise PACS or voice recognition. These tactics can maximize productivity for scheduled procedures, but managers also must be able to coordinate the unannounced or short-noticed arrivals, such as when demand for emergent interpretations may shift from 0.5 full-time employees to 10 full-time employees in a matter of minutes. It is critical to be able to ramp up and down to respond quickly to such volume fluctuation. Teleradiology offers one way to address this potential problem, if the provider can deliver consistent report turnaround times coupled with quality service, regardless of volume volatility.
Emergent Imaging Volume
At our four Sacramento area hospitals, we have reconciled the challenge of load balancing our turbulent emergent daytime and nighttime volumes in two ways. First, we made sure that our in-house daytime radiologists had the necessary tools, such as enterprise PACS and voice recognition systems, in place, as well as appropriate staff resources to monitor and navigate incoming routine and emergent imaging procedures. Second, we partnered with telerad provider Virtual Radiologic Corporation to provide nighttime emergent teleradiology interpretations and handle unplanned surges in exams needing interpretation. We can send an ever-changing number of studies for interpretation with no notice and without compromising turnaround times. This is possible because the teleradiology system automatically distributes imaging studies to a large pool of available radiologists, supported by a live 24/7 operations center.
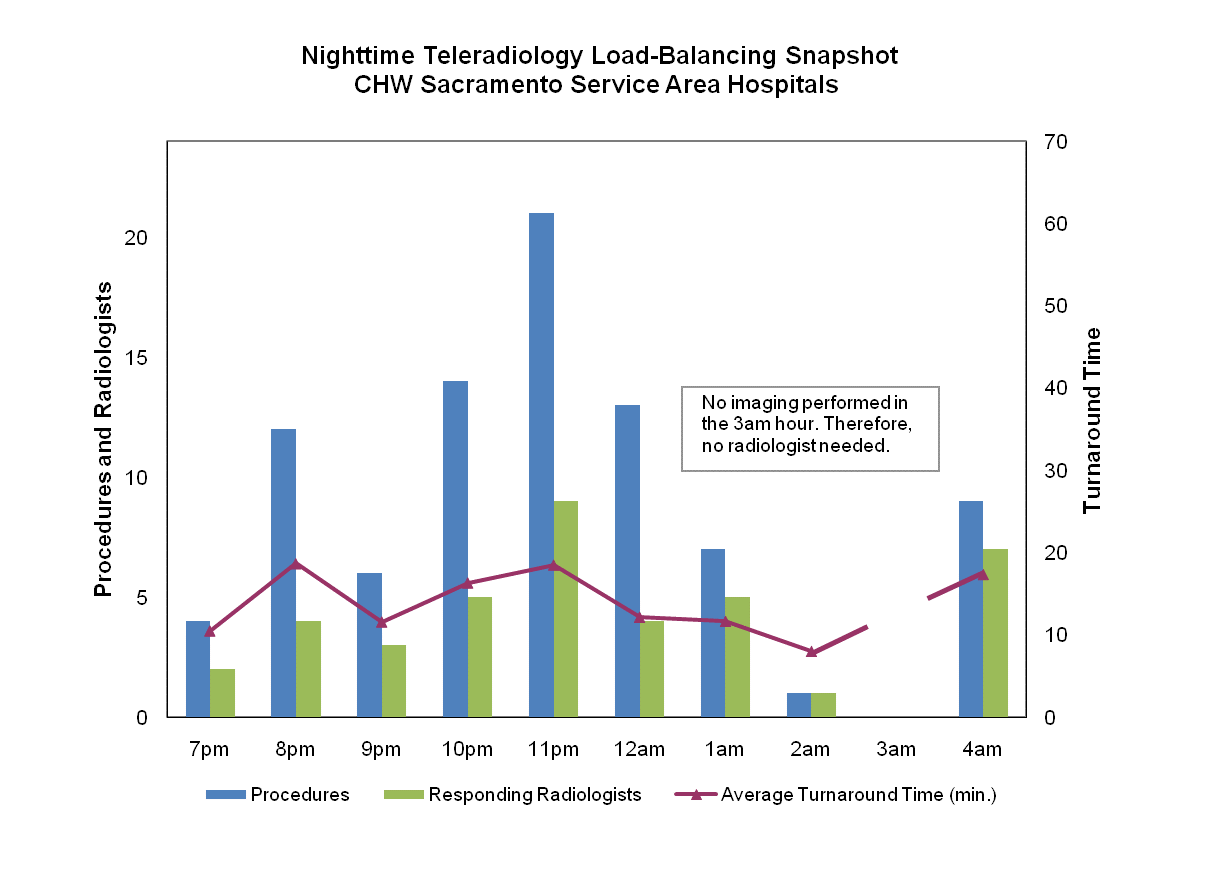
To demonstrate the load-balancing successes we achieve with teleradiology, consider the information in Figure 1, which is a typical snapshot view showing volume, the number of interpreting teleradiologists, and emergent report turnaround times for our four hospitals on one night earlier this year. Clearly, demand spiked several times during this night, particularly in the 10 pm and 11 pm hours. As demand increased, so did the number of radiologists responding. Between 11 pm and midnight, nine off-site teleradiologists read studies for our facilities, up from two earlier in the evening when there was less demand. Conversely, there were no imaging transmissions between 3 am and 4 am, yet full, instant access to the teleradiology service remained available.
If the hospital had only one radiologist on call, the doctor could have easily been overwhelmed by the number of studies and images. Turnaround times could have suffered, contributing to delays in service and to staff, physician, and patient dissatisfaction. The average turnaround time for the evening was 15.5 minutes, with no individual hourly average exceeding 19 minutes.
Our ability to balance this fluctuating demand with teleradiology support helped us to increase patient throughput by approximately 55% between 5:30 pm and 7 am with the same number of technologists and clerical staff—and without compromising quality.
What do you look for in a teleradiology partner? There are more providers in the marketplace than ever. Look for a provider that can show evidence-based performance that demonstrates well-defined load-balancing procedures and the staffing and technology to support it. Look for a teleradiology provider that can demonstrate performance in the following areas:
• An effective peer-reviewed quality assurance program with acceptable discrepancy rates.
• consistent, sustainable turnaround times;
• quality reports that provide the high-level and detailed, actionable information many ordering physicians require;
• a large, regularly scheduled network of dedicated, U.S.-based radiologists and support staff to manage any volume;
• a connected community of subspecialty radiologists capable of immediate consultation on difficult or rare cases;
• real-time navigation of all incoming imaging procedures and outgoing reports through a live, 24/7 call center (When adding staff is not an option, teleradiology support teams should free your technologists and tech aids to move on to the next patient by providing comprehensive order and technical support.);
• a robust infrastructure with bandwidth and redundancies capable of handling short-term volume spikes and long-term volume growth; and
• the ability to deliver overflow reads that support the in-house radiologists on an as-needed basis.
Without the appropriate oversight, staffing, and technological architecture, many hospitals and radiology groups are attempting to tackle a problem that is simply not manageable. Others may be relying on a teleradiology system that is incapable of performing in such a demanding environment. Therefore, when utilizing a teleradiology service, it is imperative that the provider is structured to deliver on these expectations.
Solutions that achieve and maintain a balanced workload and have a positive impact on the performance of your ED are readily available. Whether you are faced with your busiest night ever in the ED, the most complex set of imaging cases certain to bottleneck your throughput, or an urgent need for a subspecialty read, you will be in control if you utilize a teleradiology service that has mastered the load-balancing playbook.
— Marty Khatib, JD, RT(R), is the director of imaging services at Mercy San Juan Medical Center in Carmichael, Calif.
References
1. Pitts SR, Niska RW, Xu J, Burt CW. National Hospital Ambulatory Medical Care Survey; 2006 emergency department summary. Natl Health Stat Report. 2008;(7):1-38.
2. Agency for Healthcare Research and Quality. New data say uninsured account for nearly one-fifth of emergency room visits. Health and Human Services press release. July 15, 2009. Available at: http://www.ahrq.gov/news/press/pr2009/hhsuninserpr.htm.

