 March/April 2026 Issue
March/April 2026 Issue
On the Case
By Rebecca White, MD; Gilbert Lanoue, MD; Mohammad Altoos; Rola Altoos, MD; and Midhir J. Patel, MD
Radiology Today
Vol. 27 No. 2 P. 30
History
A 47-year-old woman with a remote history—at least 15 years prior—of brain tumor status postresection and ventriculoperitoneal (VP) shunt placement in Venezuela presented to the emergency department with a three-day history of headache, nausea, and vomiting. Associated symptoms included blurred vision and dizziness severe enough to precipitate near-falls. She denied fevers, chills, night sweats, and abdominal pain. Vital signs were within normal limits, and physical examination revealed no neurological deficits.
The patient reported no routine medical care prior to this presentation and no follow-up for the VP shunt since its initial placement in Venezuela. Prior medical records were unavailable for review.
Neurosurgery was consulted for further management. A nuclear medicine radiolabeled shunt study was ordered to assess VP shunt patency. This study demonstrated reflux of radiotracer into the ventricles, confirming proximal shunt patency; however, focal accumulation of radiotracer activity at the distal tip raised concern for distal obstruction. This prompted abdominal radiography and CT imaging of the abdomen and pelvis with contrast to evaluate the cause of the distal obstruction.
Findings
Figure A. Anteroposterior abdominal radiograph. The image demonstrates the shunt catheter coursing over the right hemiabdomen with the distal tip projecting over the right upper quadrant.
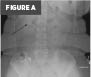
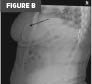
Figure B. Lateral abdominal radiograph. The image demonstrates the catheter course across the abdomen.
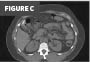
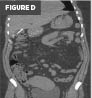
Figures C, D, and E. Axial, coronal, and sagittal CT images of the abdomen with contrast. Images demonstrate the distal shunt catheter residing within the gallbladder lumen.
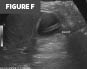
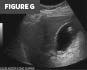
Figures F and G. Color Doppler and grayscale sonographic images. Images confirm the intraluminal position of the VP shunt catheter within the gallbladder, without wall thickening, pericholecystic fluid, or increased vascularity.
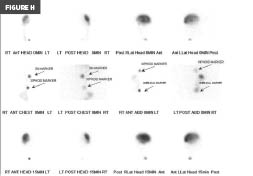
Figures H and I. Tc-99m DTPA scintigraphy images. Images demonstrate patency throughout the catheter course, with the distal catheter tip identified within an ovoid structure consistent with the gallbladder.

CT imaging revealed the distal shunt tip to be located within the gallbladder lumen (Figures C, D, and E). Importantly, there was no free intraperitoneal fluid or gas. The gallbladder wall appeared normal and intact, without pericholecystic inflammatory changes.
Given the presence of motion-related artifact on the initial CT, a gallbladder ultrasound was performed, confirming the intraluminal position of the VP shunt catheter (Figures F and G). Ultrasound further demonstrated the absence of gallbladder wall thickening or pericholecystic fluid—findings that would be expected in the setting of inadvertent catheter migration or erosion into the gallbladder.
Initial surgical planning favored cholecystectomy with shunt repositioning. However, the absence of acute cholecystitis, free intraperitoneal fluid, abdominal pain, peritoneal signs on examination, and normal liver function tests prompted a thorough literature review to investigate the possibility of intentional intracholecystic shunt placement.
Diagnosis
Appropriately positioned and functioning ventriculo-gallbladder (VG) shunt.
Discussion
First described in the mid-20th century, the VG shunt—also referred to as the ventriculo-vesicular shunt—represents an alternative cerebrospinal fluid (CSF) diversion strategy for patients with recurrent distal shunt obstructions or infections. Prior to its introduction, ventriculoatrial shunts served as the principal alternative to failed or infected VP shunts. The gallbladder is physiologically suited to serve as the distal outflow for a ventricular catheter owing to its intrinsic enzymatic capacity to metabolize CSF constituents. In fact, the gallbladder’s functional volume exceeds the daily volume of CSF production.
The published literature on VG shunts consists predominantly of case reports describing the procedure in pediatric patients requiring long-term or permanent CSF diversion. Nevertheless, a VG shunt is not a first- or second-line intervention. Standard first-line management employs a VP shunt, with the distal catheter coiling freely within the peritoneal cavity. Long-term indwelling foreign bodies such as shunt catheters are inherently susceptible to complications including infection, mechanical failure, fracture, and migration. Surgical revision and replacement carry cumulative patient risk. Furthermore, adhesions and scar tissue formation not only may obstruct the catheter tip but also can entrap adjacent structures. Despite these limitations, the VP shunt remains preferred over the VG shunt; VG shunting is considered a true “last resort” due to its associations with shunt-imposed biliary dysfunction, malabsorption, and infection.
Although no formal medical records are available in this case to confirm intentional VG shunt placement, the imaging findings—corroborated by a focused literature review—are reassuring for deliberate intracholecystic catheter placement. Recognizing this uncommon but established surgical technique in the context of an acute presentation was critical to avoiding unnecessary operative intervention. After three days of conservative management, the patient’s symptoms resolved and she was safely discharged with outpatient neurosurgery follow-up arranged.
— Rebecca White, MD, is a diagnostic radiology resident at AdventHealth in Orlando, Florida.
— Gilbert Lanoue, MD, is a diagnostic radiology resident at AdventHealth.
— Mohammad Altoos is a medical student at Valencia College in Orlando, Florida.
— Rola Altoos, MD, is an attending radiologist at AdventHealth.
— Midhir J. Patel, MD, is an attending radiologist at AdventHealth.
Resources
1. Bue EL, Morello A, Bellomo J, et al. Ventriculoatrial shunt remains a safe surgical alternative for hydrocephalus: a systematic review and meta-analysis. Sci Rep. 2024;14(1):18460.
2. Demetriades AK, Haq IZ, Jarosz J, McCormick D, Bassi S. The ventriculocholecystic shunt: two case reports and a review of the literature. Br J Neurosurg. 2013;27(4):505-508.
3. Hosainey SAM, Lykkedrang BL, Meling TR. Long-term risk of shunt failure after brain tumor surgery. Neurosurg Rev. 2022;45(2):1589-1600.
4. Porto Junior S, Ramos JVB, da Cunha BLB, et al. Ventriculo-gallbladder shunt. J Clin Neurosci. 2024;121:83-88.
5. West KW, Turner MK, Vane DW, Boaz J, Kalsbeck J, Grosfeld JL. Ventricular gallbladder shunts: an alternative procedure in hydrocephalus. J Pediatr Surg. 1987;22(7):609-612.

