E-News Exclusive
Chuck Norris Lawsuit Claims MRI Agent Poisoned His Wife
By Bruce Y. Lee
Yes, I am writing about a Chuck Norris fight.
[Recently], the martial artist and his wife, Gena Norris, filed a lawsuit in the San Francisco Superior Court, alleging that Gena was poisoned by gadolinium-based contrast agents (GBCAs) used for MRI scans. Defendants include GBCA manufacturers such as McKesson Corporation, Bracco S.p.A., and ACIST Medical Systems Inc.
As Ron Leuty described for the San Francisco Business Times, the claim is that in late 2012 Gena Norris began experiencing heart pounding and an “intense burning” in her body after undergoing three MRI scans over an eight-day period. Despite multiple visits to the hospital, her symptoms continued to worsen, until she had to leave Texas and travel as far as China to receive controversial alternative treatments such as chelation therapy and stem cell treatments.
Although reportedly her symptoms have since improved, she still has not returned to normal, as periodically she suffers cramps in her hands and “It feels like a hot poker is going up my spine.” Leuty included a quote from Gena Norris: “I am broken. I don’t blame the doctors at all, because [companies] have been keeping things hidden and in the shadows.”
Egad, can gadolinium (often abbreviated as GAD) really cause all this? Gadolinium is a heavy metal that alone could be highly toxic to humans. However, MRI contrast agents include a chelating agent bound to gadolinium that is supposed to prevent this toxicity.
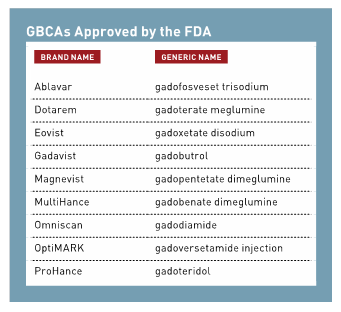
Radiologists have used GBCAs for MRIs since 1988. The thought is that after the MRI this combination of gadolinium and chelating agent would be rapidly and completely excreted from the body through urine.
However, studies summarized by a review article in Biometals suggest that this is not always the case. Radiologists avoid giving the contrast agents to patients with kidney failure because the patient may not be able to excrete all of the contrast agent and worsening kidney failure (nephrogenic systemic fibrosis) may result. But, as summarized in the review, studies have found that gadolinium may accumulate in different parts of the body, such as the bone, brain, and kidneys, even if the kidneys are functioning normally. In fact, in 2015, the FDA issued a safety announcement that it was investigating the risk of GBCAs building up in the brain. Although the FDA did issue a follow-up announcement this year stating that they have yet to find enough scientific evidence that gadolinium accumulation in the brain can adversely affect health, the thought that something else is sitting in the brain besides thoughts and limericks may be a bit disconcerting.
Indeed, the review article mentioned cell culture and pig studies that have shown how GBCAs can damage kidney cells. There’s also a case report of a 56-year-old woman who developed kidney failure after getting a GBCA and two case reports of patients suffering pancreatitis. Studies in mice have demonstrated that GBCAs may result in decreases in white blood cell counts, increases in inflammatory cytokines, and changes in liver cells. And injecting rats with GBCA seemed to produce neurological problems such as tremor, difficulties with coordination and balance, and behavioral problems. Moreover, in a 2009 issue of the American Journal of Neuroradiology, radiologists Ferdinand Hui, MD, and Mark Mullins, MD, PhD, reported on a patient who developed encephalopathy after receiving a GBCA for an MRI.
Of course, case studies and animal studies are not the same as more extensive human studies, and GAD can play a crucial beneficial role, helping doctors better find and evaluate abnormalities. So don’t roundhouse kick GBCAs just yet. However, all of this suggests that a closer look at the safety of GBCAs (including more rigorous scientific studies) may be necessary.
Will the Norris lawsuit be successful, do the claims have merit, and will more claims of GBCA toxicity emerge as a result of Norris bringing more attention to GBCAs? Time and the details of what actually happened to Gena Norris will tell.
— Bruce Y. Lee is a contributor at Forbes.

