A Surprise Within a Surprise
History and Course of Illness
A 70-year-old male with a history of hypertension presented to the emergency department with acute-onset right upper quadrant pain described as constant and sharp. The initial workup included a CT of the abdomen and pelvis with IV contrast. Imaging prompted surgical intervention.
Findings
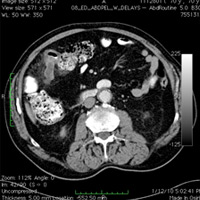
Contrast-enchanced CT of the abdomen and pelvis demonstrated a dilated, tubular blind-ending structure arising from the terminal ileum. Associated mesenteric inflammatory stranding was noted. A normal appendix was identified.
Diagnosis
Carcinoid tumor arising within an inflamed Meckel’s diverticulum (MD)
Discussion
Meckel’s diverticulum (MD) is the most common congenital anomaly of the gastrointestinal tract, with prevalence approaching 2%. MD is essentially the failure of omphalomesenteric duct regression.
A Meckel’s diverticulum containing a carcinoid tumor is even more uncommon, with only 111 reported cases in the literature.1 Neoplasms such as benign lipomas,2 adenocarcinomas,2,3 gastrointestinal stromal tumor,4 and signet-ring cell adenocarcinomas are also found5 within MD on rare occasion. Clinical features range from an acute abdomen with severe gastrointestinal hemorrhage and/or perforation to chronic symptoms of obstruction and anemia. Workup may include barium studies, abdominopelvic CT or MRI, laparotomy, Meckel’s scan (99-m-technetium-pertechnetate), and/or digital subtraction angiography of the superior mesenteric artery, which in 10% of cases leads to the discovery of a vitelline artery supplying the MD.
Treatment involves diverticulectomy and appendectomy with primary small-bowel anastomosis. MD tends to be more symptomatic in men. Surgical treatment of carcinoid tumors is generally based on the size and extent of the primary lesion. For solitary lesions smaller than 1 cm without mesenteric adenopathy, segmental resection is considered satisfactory. For larger or multiple lesions, segmental bowel and mesenteric excision is favored. Patients with locally staged carcinoids of the small bowel have an overall survival rate of 75%, which coincidentally approximates the statistics for carcinoid found within a Meckel’s diverticulum.1
— Dhiraj Rajkumar, MD, is a radiology resident at St. Barnabas Medial Center in Livingston, N.J.
— Cornelius S. McCarthy, MD, is president of Imaging Consultants of Essex and a member of the radiology staff at St. Barnabas Medical Center.
 |
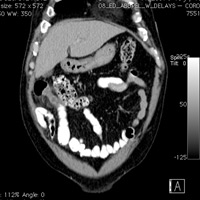 |
| Figure 1 — Axial CT revealing inflamed Meckel’s diverticulum | Figure 2 — Sagittal CT revealing inflamed Meckel’s diverticulum arising from ileum |
 |
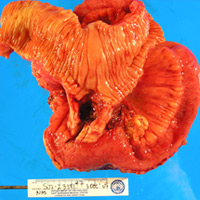 |
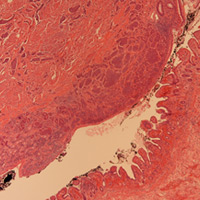
| Figure 3 — Lower right shows small bowel/Meckel’s diverticulum. Upper left shows carcinoid. | Figure 4 — Gross specimen of small-bowel Meckel’s diverticulum |
REFERENCES
- Schwartz SI, Fischer JE, Daly JM, Shires GT, Galloway AC. Principles of Surgery. 7th ed. New York: McGraw-Hill; 1998.
- Dumper J, Mackenzie S, Mitchell P, Sutherland F, Quan ML, Mew D. Complications of Meckel’s diverticula in adults. Can J Surg. 2006;49(5):353-357.
- Green M, Oratz R, Muggia FM. Carcinoid syndrome from a tumor of Meckel’s diverticulum. Am J Med. 1987;83(1):184-186.
- Hager M, Maier H, Eberwein M, et al. Perforated Meckel’s diverticulum presenting as a gastrointestinal stromal tumor: A case report. J Gastrointest Surg. 2005;9(6):809-811.
- Lippe P, Berardi R, Latini L, Bracci R, Cellerino R. Severe prognosis of signet-ring cell adenocarcinoma occurring in Meckel’s diverticulum. Ann Oncol. 2001;12(2):277.
ON THE CASE submission requirements
- Cases should have clinical relevance and clear radiological findings.
- Sections should include a title, history and course of illness, findings, diagnosis, and discussion.
- Maximum word limit should not exceed 800. At least three references are recommended.
- Cases may be submitted from any radiological subspecialty and imaging modality.
- Figures must be high-quality JPEG or TIFF images and labeled for ease of reference. Please keep images in their native format, without the addition of arrows or other means of highlighting the key findings.