Splenium Lymphoma
History and Course of Illness
A 68-year-old man with a history of prostate cancer presented to his primary care physician after two weeks of “intense” short-term memory loss. He also reported generalized decline in his activity level during the preceding few months and accompanying weight loss. Physical and neurological examination were both unremarkable. A lesion found on an outpatient MRI prompted emergent admission. A biopsy of the brain lesion was performed, followed by the patient’s transfer to the neurosurgical ICU.
Findings
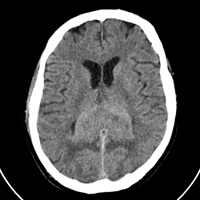
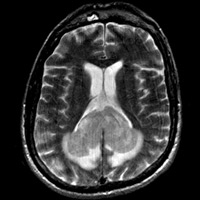
Noncontrast CT of the head demonstrates a relatively hyperdense, expansile mass within the splenium of the corpus callosum. A mild rim of hypodensity surrounds the margins of the mass, extending into the parieto-occipital white matter (WM). T1-weighted image (T1WI) reveals a mass that is isointense to gray matter (GM) and isointense to mildly hyperintense on T2WI. The fluid-attenuated inversion recovery (FLAIR) sequence confirm the presence of a hyperintense, expansile mass infiltrating the splenium, with only minimal contiguous hyperintensity within the WM, presumably vasogenic edema. Furthermore, T2WI and FLAIR sequences confirms the presence of internal cystic degeneration. Postcontrast T1WI reveals a strongly enhancing, partially necrotic mass. Abnormal restricted diffusion verified by the trace images and corresponding apparent diffusion coefficient (ADC) map.
Diagnosis
Diffuse large B-cell lymphoma. CD20 positive; Glial Fibrillary Acidic Protein negative; Ki-67 immunostain (MIB-1 proliferation index) approximately 70%.
Discussion
Primary central nervous system lymphoma (PCNSL) is believed to be secondary to the dysfunction of suppressor T cells, ultimately leading to B-cell lymphocytic neoplasm. The majority of these lesions are supratentorial, located deep within the periventricular WM (along ependymal surfaces), deep gray nuclei, or arising from the corpus callosum (as illustrated herein). PCNSL can arise de novo or in patients who are immunocompromised (eg, diagnosed with AIDS or receiving an organ transplant). Projected estimates of incidence suggest that lymphoma may become the most common primary brain malignancy, given the prevalence of AIDS.1
Imaging of PCNSL is variable depending on a patient’s immune status. Lesions are generally hyperdense on noncontrast CT. On T1WI, lymphoma tends to be isointense or hypointense to GM. Appearance on T2WI is variable, with nearly 50% of lesions demonstrating either hypo- or hyperintensity. Strong enhancement is usually the case in immunocompetent individuals, whereas more heterogeneous (ie, rim-enhancing) lesions are characteristic of immunodeficiency. Johnson et al demonstrated a statistically significant correlation between a higher degree of necrosis histologically and hyperintensity on T2WI; imaging characteristics, lesion location, lesion size, and proclivity to harbor necrosis are all altered in the immunocompromised patient.2
For a mass lesion replacing or invading the corpus callosum, the primary differential consideration is high-grade astrocytoma (ie, glioblastoma). T1WI, T2WI, and gadolinium-enhancement patterns may overlap with PCNSL. Diffusion-weighted imaging, fortunately, is a dependable means of distinguishing between the two entities. Owing to their dense cellularity (high nuclear/cytoplasmic ratio), lymphoma demonstrates profound decrease in ADC values. In a study investigating 27 patients with glioblastoma multiforme (GBM), five patients with low-grade astrocytoma, and nine patients with primary lymphoma infiltrating the corpus callosum, water diffusivity and the ADC ratio of GBM and low-grade astrocytic tumor differed significantly from lymphoma, allowing for reliable differentiation between tumor types.3
Dynamic susceptibility contrast-enhanced MR perfusion has emerged as an additional tool to aid in distinguishing between PCNSL and glioblastoma. MR perfusion essentially quantifies the degree of relative cerebral blood volume (rCBV) within a lesion compared with normal-appearing WM. Similar to the principle behind the observed restricted diffusion, the dense cellularity of PCNSL is thought to limit the extent of intralesional vascularity and subsequent contrast leakage. Liao et al demonstrated that the maximum rCBV ratio of lymphoma was 1.72+/-0.59 compared with high-grade astrocytoma, which equaled 4.86+/-2.18.4
Histology confirmed large B-cell non-Hodgkin lymphoma with a markedly elevated proliferation index (Ki-67 expression). Ki-67 is a nuclear antigen protein present in all actively dividing cells and is utilized to assess tumor growth fraction. With respect to diffuse large B-cell lymphoma, a Ki-67 proliferation index of 70% has been found to discriminate between patients with good or bad prognosis; a cutoff value of 45% could be used to help differentiate indolent from aggressive disease.5
— Rahul V. Pawar, MD, DABR, is an attending neuroradiologist at Saint Barnabas Medical Center in Livingston, N.J.
 |
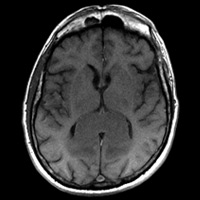 |
| Figure 1 — Noncontrast head CT shows expansile, hyperdense mass within the splenium. | Figure 2 — T1WI shows lymphoma to be isointense to GM. |
 |
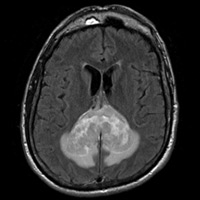 |
| Figure 3 — Mass is iso- to mildly hyperintense to GM on T2WI, with internal foci of cystic degeneration/necrosis. | Figure 4 — FLAIR sequence shows hyperintense lesion with areas of internal cystic degeneration/necrosis and mid surrounding vasogenic edema. |
 |
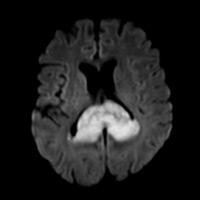 |
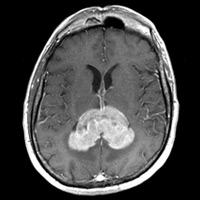
| Figure 5 — Postcontrast T1WI shows strong, heterogenous enhancement and partially necrotic mass. | Figure 6 — Trace diffusion images with hyperintense signal |
 |
|
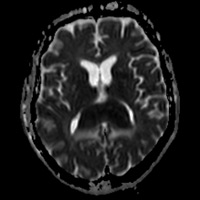
| Figure 7 — Apparent diffusion coefficient map with hypointense signal |
REFERENCES
- Yousem DM, Grossman RI. Neuroradiology: The Requisites. 3rd ed. Philadelphia: Mosby; 2010:93-94.
- Johnson BA, Fram EK, Johnson PC, Jacobowitz R. The variable MR appearance of primary lymphoma of the central nervous system: Comparison with histopathology features. AJNR Am J Neuroradiol. 1997;18(3):563-572.
- Horger M, Fenchel M, Nägele T, et al. Water diffusivity: Comparison of primary CNS lymphoma and astrocytic tumor infiltrating the corpus callosum. AJR Am J Roentgenol. 2009;193(5):1384-1387.
- Liao W, Liu Y, Wang X, et al. Differentiation of primary central nervous system lymphoma and high-grade glioma with dynamic susceptibility contrast-enhanced perfusion magnetic resonance imaging. Acta Radiol. 2009;50(2):217-225.
- Broyde A, Boycov O, Strenov Y, Okon E, Shpilberg O, Bairey O. Role and prognostic significance of the Ki-67 index in non-Hodgkin’s lymphoma. Am J Hematol. 2009;84(6):338-343.
ON THE CASE submission requirements
- Cases should have clinical relevance and clear radiological findings.
- Sections should include a title, history and course of illness, findings, diagnosis, and discussion.
- Maximum word limit should not exceed 800. At least three references are recommended.
- Cases may be submitted from any radiological subspecialty and imaging modality.
- Figures must be high-quality JPEG or TIFF images and labeled for ease of reference. Please keep images in their native format, without the addition of arrows or other means of highlighting the key findings.