So It’s a Mass — Let’s Take It a Step Further
History and Course of Illness
A 63-year-old woman underwent a routine CT scan of the abdomen and pelvis due to pain. No obvious radiographic etiology for her pain was found. However, another finding was made, prompting deeper concern, especially given her age and significant pack-year history of smoking. To further characterize the lesion, MRI was performed with multiphase acquisition.
Findings
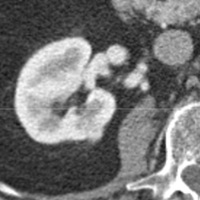
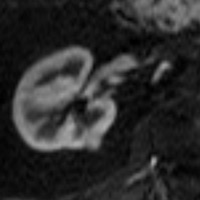
Contrast-enhanced CT during the corticomedullary phase demonstrated a 1.1-cm homogeneously enhancing, well-circumscribed lesion arising from the posteromedial cortex of the right kidney (Figures 1 and 2). No intralesional calcifications, hemorrhage, or necrosis was appreciated. On T2-weighted imaging (Figure 3), the lesion was mildly hypointense relative to normal cortex. On precontrast T1-weighted imaging (Figure 4), the lesion was isointense, demonstrating strong, avid enhancement during the corticomedullary (Figure 5) and nephrographic phases (Figure 6).
Diagnosis
Renal cell carcinoma (RCC), clear-cell subtype
Discussion
RCC constitutes a small fraction of all adult malignancies but compromises greater than 90% of all renal neoplasms. Older individuals are affected disproportionately, with a slight male predilection. Perhaps due to surges in advanced imaging acquisition, RCC is being detected at earlier stages. Numerous risk factors are implicated, including, but not limited to, advanced age, tobacco use, chemical exposure, long-term hemodialysis, strong family history of RCC, history of prior renal radiation, and hereditary syndromes (eg, von Hippel-Lindau syndrome, tuberous sclerosis).
In the present day, nephron-sparing surgical techniques are remarkable, allowing for preservation of significant renal function. Even patients with advanced stages of RCC (eg, Robson stage III) have benefited from evolution of surgical practice.1
Pathologists know several subtypes of RCC, and currently imaging has progressed to a point where histology may be predictable. Clear-cell (conventional) RCC is by far the most common subtype (70%), with a five-year survival approaching 60%. Papillary RCC is the second most common subtype, with five-year survival approaching 90%. Collecting duct RCC is the least common subtype (less than 1%) with a comparatively dismal prognosis: Five-year survival is less than 5%.2 Negative prognostic factors include paraneoplastic syndromes (eg, anemia, hypercalcemia, hepatic dysfunction, thrombocytosis, fever, weight loss) and obesity.3
On contrast-enhanced CT, enhancement patterns are reported to be the most useful parameter in differentiating between subtypes. During the corticomedullary and excretory phases, clear-cell RCC typically exhibits the strongest enhancement, likely a function of its rich vascular network and alveolar architecture. Aggressive features such as hemorrhage and/or necrosis also portend lower five-year survival rates, more commonly seen with clear-cell and collecting duct RCC. The same study found that calcifications herald a slightly better prognosis and are often seen with the papillary subtype.2 With both CT and MRI, the nephrographic phase of enhancement is considered the most diagnostic for lesion identification and differentiation between subtypes.
Clear-cell RCC is typically hypointense or isointense on T1-weighted imaging and isointense to hyperintense on T2-weighted imaging. Avid enhancement postgadolinium administration is generally the rule, given this subtype’s intrinsic hypervascularity. Signal dropout on opposed-phase MR images may signify the presence of microscopic fat. Conversely, papillary RCC is a comparatively hypovascular tumor, demonstrating only mild enhancement. T2-weighted signal may overlap with clear-cell RCC, since both may have internal hemorrhage and/or necrosis, occasionally diminishing its utility in differentiation. Interestingly, papillary RCC is also more frequently associated with hereditary syndromes and exhibits multifocality and bilaterality.4
For the resident in training or even a busy radiologist several years into practice, applying advanced imaging techniques and bringing imaging characterization to a higher level can appear daunting and, at times, unnecessary. However, it is important to remember that as the radiology field moves forward, so do the expectations from our referring colleagues. The goal of image interpretation should not be limited to identifying the lesion and offering a differential diagnosis. Our imaging tools enable us to take it several steps further and make us indispensable to our referral base, hospital, and—most importantly—our patients. In the case of RCC, histologic and radiologic subtyping can be predictors of clinical behavior, prognosis, and response to treatment (ie, high resistance of metastatic non–clear-cell RCC to interleukin-based treatment).5
— Rahul V. Pawar, MD, is a board-certified diagnostic radiologist completing a fellowship in neuroradiology at New York University Langone Medical Center.
— Shamkant Mulgaonkar, MD, is chief of the renal and pancreas transplant division of Saint Barnabas Health Care System in Livingston, N.J., and past president of the Transplant Society of New Jersey.
 |
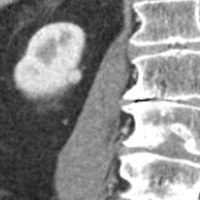 |
| Figures 1 and 2 — Contrast-enhanced CT during the corticomedullary phase demonstrates a 1.1-cm homogeneously enhancing, well-circumscribed lesion arising from the posteromedial cortex of the right kidney. | |
 |
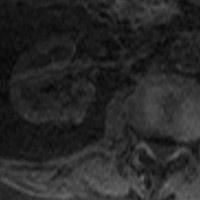 |
| Figure 3 — On T2-weighted imaging, the lesion is mildly hypointense relative to normal cortex. | Figure 4 — On precontrast T1-weighted imaging, the lesion is isointense. |
 |
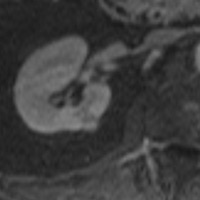 |
| Figure 5 — Contrast-enhanced MR image demonstrates strong, avid enhancement during the corticomedullary phase. | Figure 6 — Contrast-enhanced MR image shows strong, avid enhancement during the nephrographic phase. |
REFERENCES
- Ergen FB, Hussain HK, Caoili EM, et al. MRI for preoperative staging of renal cell carcinoma using the 1997 TNM classification: Comparison with surgical and pathologic staging. AJR Am J Roentgenol. 2004;182(1):217-225.
- Kim JK, Kim TK, Ahn HJ, Kim CS, Kim KR, Cho KS. Differentiation of subtypes of renal cell carcinoma on helical CT scans. AJR Am J Roentgenol. 2002;178(6):1499-1506.
- Calle EE, Rodriguez C, Walker-Thurmond K, Thun MJ. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med. 2003;348(17):1625-1638.
- Prasad SR, Humphrey PA, Catena JR, et al. Common and uncommon histologic subtypes of renal cell carcinoma: Imaging spectrum with pathologic correlation. Radiographics. 2006;26(6):1795-1806.
- Upton MP, Parker RA, Youmans A, McDermott DF, Atkins MB. Histologic predictors of renal cell carcinoma response to interleukin-2-based therapy. J Immunother. 2005;28(5):488-495.
ON THE CASE submission requirements
- Cases should have clinical relevance and clear radiological findings.
- Sections should include a title, history and course of illness, findings, diagnosis, and discussion.
- Maximum word limit should not exceed 800. At least three references are recommended.
- Cases may be submitted from any radiological subspecialty and imaging modality.
- Figures must be high-quality JPEG or TIFF images and labeled for ease of reference. Please keep images in their native format, without the addition of arrows or other means of highlighting the key findings.